
*Disclaimer: the information on this site is intended as general information only and does not serve as personal medical or therapeutic advice. Use with caution and consult a medical professional familiar with your case beforehand.
If you work in pediatric therapy, OP neuro rehab, acute care or inpatient rehabilitation settings you will most likely find yourself needing to do elements of a neuro screen during your evaluations. Even if you decided well before you graduated PT school that you would never work with neurologic patients and you were going to dedicate your career to sports and orthopedic rehab you will undoubtedly encounter scenarios in which you need to do at least some elements of the neurologic screen. If you haven’t ever encountered this, there is a good chance you missed out on an important opportunity to screen for neurologic impairments in at least some of your patients. Unlike a neurologic examination/evaluation that many of us perform on a patient with a known neurologic condition, I consider the neurologic screen to be a tool that helps inform therapists whether the nervous system may be involved in a patient that does not have a known neurologic condition, to help differentially diagnose an impairment that may be undiagnosed or unrecognized or to provide valuable information about nervous system function that could impact the plan of care.
Despite our comprehensive education in physical therapy school, I bet all practicing therapists have been faced with the reality that unless you use a particular area of knowledge or skill pretty regularly, you lose your familiarity and comfort with it pretty quickly. Nothing to be ashamed of, we can’t be experts in everything, but having a basic comfort with the elements of the neuro screen will go a long way in helping therapists create a more comprehensive and effective plan of care and also help identify patients that need to be referred back to their doctors for more testing or medical care. Also, so it doesn’t seem as though I’m just picking on the ortho therapists out there, Neuro Folks, if you aren’t screening your patients for and addressing their orthopedic problems, you’re missing an important piece also!
What’s in a Neuro Screen?
**Alright, quick forewarning here that this is not a completely comprehensive outline of every possible neurologic test you can perform on your patient. You can find that in your neuro rehab textbook.
Performing a good neuro screen requires both an understanding of the purpose of each neurologic test and measure and an ability to determine when to use what test. As a student physical therapist or novice clinician, the clinical reasoning process often involves administering a lot of subjective and objective outcome measures, looking at the results for anything that suggests an impairment or functional limitation then deriving a PT diagnosis and plan of care based on the results of those tests. As clinicians gain experience they often draw very heavily on their understanding of injury and disease and their past patient experiences to make hypotheses that allow them to immediately narrow down the tests and measures they believe will be most pertinent.
If you aren’t as comfortable with the myriad of neurologic screening tools out there and haven’t worked with that population of patients for a long time or very often, use the information below as a jumping off point for selecting tests that should help you recognize how the neurologic and neuromuscular systems are impacted in your patients.
Should I throw the kitchen sink at them?
If you are lucky enough to work in a magical PT clinic where you can spend 2 hours evaluating your patient on the first day then by all means, have at it. If you don’t work in inpatient rehab and you don’t happen to work in a setting that allows for much longer 1:1 sessions with the therapist then you need to be selective and judicious when structuring your exams.
Scenario 1: Patient arrives with a known neurologic diagnosis (Stroke, Multiple Sclerosis, Neuropathy, etc.)
Approach: Use your knowledge about the patient’s injury or condition and the impairments and activity/participation limitations commonly associated with that injury/condition to select your tests/measures. For example, if your patient has neuropathy you would expect that motor and/or sensory systems may be affected so sensation and strength testing would be appropriate. If your patient had a stroke, you might expect changes in muscle tone as well as strength and sensation so you would screen these areas.
Because you do not have time to perform every test in the book, focus on the elements that provide information that will impact your treatment and prognosis. For example, reflex testing certainly provides valuable information about the state of the nervous system following a stroke but if the results don’t change your plan of care then they wouldn’t be my top priority.
Scenario 2: Patient arrives with a known diagnosis that you would not consider to be neurologic in nature but their history or your observation suggests the neurologic system could be contributing to their complaints
Approach: Something in your subjective or objective exam has prompted you to think that this could be neurologic in nature. In this scenario I would start by selecting tests that point to abnormalities in neurologic function such as sensation testing which could point to a dermatomal pattern of sensation loss, for example, coordination testing which can indicate cerebellar involvement, reflex testing which can help distinguish between an upper or lower motor nerve disorder, myotome testing which can indicate spinal nerve involvement or pathologic reflexes like Babinski or Hoffman’s that indicate loss of cortical inhibition and an upper motor nerve lesion.
Scenario 3: Patient arrives with a known neurologic diagnosis but your well-honed spidey-senses suspect they could have been misdiagnosed or there could be a secondary problem happening
Approach: What about this patient’s presentation has led you to believe their is more to this picture than the diagnosis they walked in with? Use this information to select your tests and measures. For example, I once evaluated a patient who had been treated for Guillain Barre Syndrome in the hospital and inpatient rehab and came to my outpatient clinic about 5 months later. On initial evaluation they presented with severe extensor tone and spasticity in the right lower extremity. This gave me pause because GBS is a lower motor neuron disorder while spasticity is an upper motor neuron sign. This finding prompted me to examine the patient further and refer them for more imaging which revealed they had been misdiagnosed and actually had either Transverse Myelitis or Multiple Sclerosis.
In these cases it is a good time to whip out your cranial nerve screens, tone assessments, pathological reflex testing, deep tendon reflex testing, coordination testing and vestibular testing among others to see if you can garner additional information that may indicate the patient should be referred back to their provider for further testing.
Many Tests to Choose From
Now that you have an idea of how to select what body structure/function you want to examine, here is a list of some helpful tests and measures that you can use to inform your plan of care. Please note this list does not include functional outcome measures that assess things like balance, gait or functional strength as I consider those to have a different purpose than a neurologic screen.
Cranial Nerve Screen
Purpose: used to identify lesions of the cranial nerves which can help localize pathology, identify areas that may impact patient response to therapy and recovery or prompt a referral to another provider for treatment.
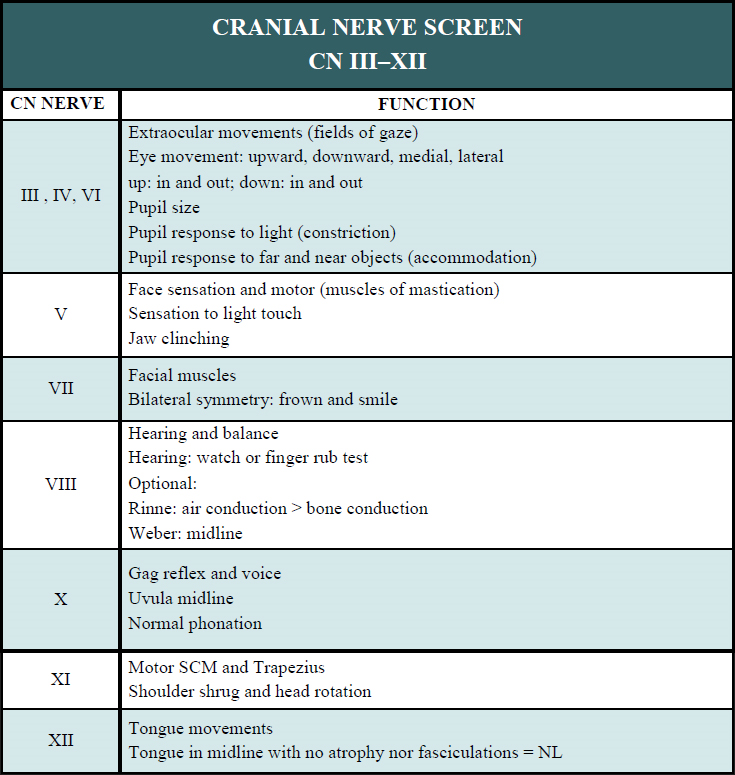
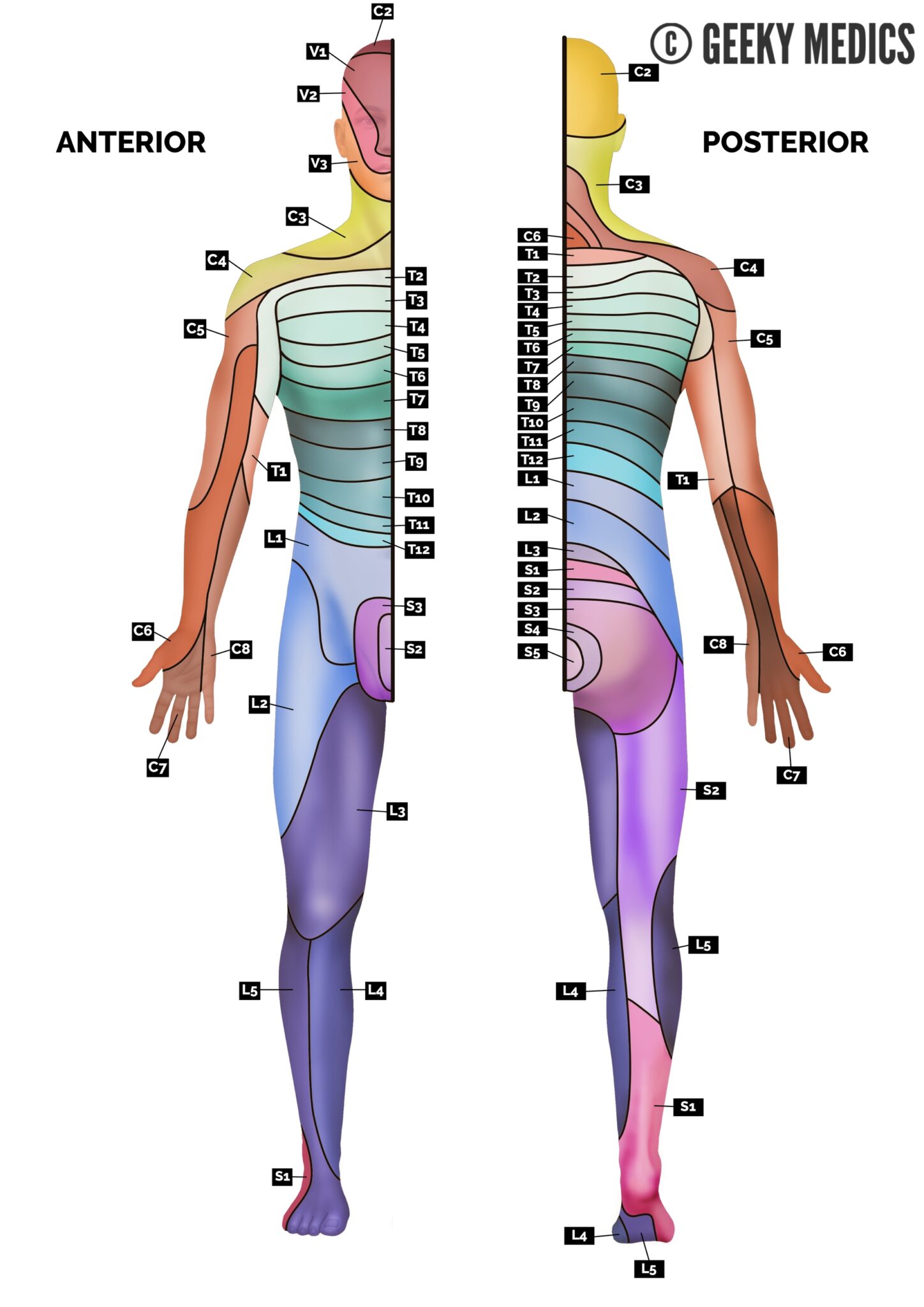
Sensory Screen:
Purpose: localize lesion, assess protective sensation, monitor the extent of neurologic recovery or disease progression; prognosticate functional outcomes
Basic sensory screen for impairments in light touch, sharp/dull, temperature and vibration can indicate location of lesion:
- Dermatomal pattern of sensory loss: indicates which spinal levels and tracts are involved
- Light touch: Ventral Spinothalamic Tract of spinal cord
- Pain (pin prick): Lateral Spinothalamic Tract of spinal cord
- Temperature: Lateral Spinothalamic Tract of spinal cord
- Proprioception: Dorsal Column of spinal cord
- Vibration: Dorsal Column of spinal cord
- Peripheral nerve distribution: indicates an injury or lesion to a particular peripheral sensory nerve
- Stocking glove pattern: usually consistent with peripheral neuropathy in which nerves are affected based on length of axon and not specific branches of nerves
- Larger areas affected on one side such as entire leg, arm, face: often points to upper motor nerve lesions involving multiple levels of the spinal cord or the sensory cortex of the brain
Cortical Sensory Testing assesses the function of the sensory association areas of the parietal lobe
- Stereognosis
- Graphesthesia
- Two point discrimination
- Localization of touch
**Clinical pearl: if you observe a patient walking unsteadily with wide base of support, possibly stomping the ground they may have a sensory ataxia caused by loss of sensation in their feet and legs. Sensation testing should help pick this up and symptoms will worsen significantly in the dark or with eyes closed.
Reflex Testing
Purpose: Deep Tendon Reflexes: assesses muscle stretch reflex and can be localized to specific nerve roots. Hyperreflexia can indicate an upper motor nerve lesion while hypo– or arreflexia can indicate a lower motor nerve lesion
- Pathologic Reflexes
- Hoffman’s Reflex: positive Hoffman’s sign (adduction and flexion of the thumb and flexion of the index finger) is suggestive of cortocospinal tract dysfunction in the cervical spinal cord
- Babinski: positive Babinski (extension of the great toe and splaying of the other toes) is suggestive of a corticospinal tract dysfunction
- Clonus: rhythmic and oscillating stretch reflex, form of hyperreflexia and indicative of an upper motor neuron lesion
Muscle Tone Assessment
Purpose: Assess the muscle’s response to passive stretch. Lower motor neuron lesions reduce muscle tone while upper motor lesions increase muscle tone
- Hypertonicity: umbrella term that refers to an increased resistance to passive stretch
- Includes spasticity, rigidity, dystonia, co-contraction, clonus
- Spasticity: specifically refers to velocity-dependent resistance to passive stretch
- Can measure with the Modified Ashworth Scale or the Tardieu
Coordination Testing
Purpose: usually considered to be a window into cerebellar function so abnormalities in these tests are concerning for cerebellar dysfunction.
-
- Rapid Alternating Movement: alternating pronation/supination or ankle plantarflexion/dorsiflexion–the cerebellum controls the ability to perform one movement quickly followed by its opposite. Impairment in this function is called dysdiadochokinesis (if you can spell this word correctly without looking it up, you are my hero).
- Finger to Nose: measures upper extremity coordination. During this test you may observe
- Dysmetria: misjudging the target (hypo vs hypermetric movements)
- Intention tremor
- Dyssynergia: refers to breakdown of movement, often see the movement broken in to several smaller movements
- Ataxia: refers to abnormal coordination of movement
- Heel to Shin: lower extremity coordination, may be dysmetric (missing target) or generally ataxic
**Clinical pearl: be aware that vision, executive function, cognition, strength and motor control can all play a role in being able to perform these coordination tests well and may confuse the results. Speeding up the movement can unmask coordination impairments
Myotome Testing
Purpose: Weakness is a common complaint in patients receiving physical therapy and may be due to numerous causes. Keep your eye out, however, for patterns of weakness that fall into a myotome pattern as this indicates spinal nerve involvement.
Vestibular and Oculomotor Screen
These tests are most often performed in the context of complaints of dizziness or disequilibrium and in patients with a known neurologic condition. However, if you have a familiarity with some of these tests you may be able to pick up on an issue that may be pertinent to their care and need further evaluation by a specialist. There is a whole litany of tests available to you to differentiate between possible causes of symptoms but these tests may help to at least determine if more in depth assessment is warranted.
Oculomotor Screen: these impairments may manifest as blurry vision, double vision, difficulty reading, impaired eye movements, dizziness, headaches, etc.
-
- Smooth pursuit: measures the eyes ability to smoothly track a moving object while the head remains in place. Also allows assessment of strength and function of the ocular muscles. Saccadic intrusions, meaning the movement is broken down into several smaller movements suggests central pathology.
- Saccades: the ability of the eye to move quickly and accurately from one target to another. Impairments typically suggest cerebellar disorder
- Convergence: the ability to adduct the eyes and view a near-target object without double vision. Normal convergence is 6-10cm. Doubling of vision before 10cm can be suggestive of a concussion, a cerebellar or brainstem injury or an impairment in eye muscle function
Vestibular Screen: these impairments are often accompanied by dizziness, vertigo, disequilibrium, falls, nausea, disorientation, feeling like you or the world is moving
-
- Vestibular-Ocular Reflex (VOR): the ability to maintain eyes locked on an unmoving target while the head is moving. Use a metronome set at 2Hz and have patient perform oscillations of the head in the sagittal and then transverse plane about 30 deg to each side while locking eyes on a small target about arm’s length away. If they experience symptoms of dizziness, nausea or headache, double vision or blurring then this indicates likely VOR impairment.
- Head Impulse Test: failure to maintain eyes locked on therapist’s nose while quickly turning the head to one side suggests peripheral vestibular dysfunction.
- VOR cancellation: reflects the ability to suppress VOR and turn eyes and head in same direction at same rate. Normal: eyes maintained in center of orbit while head and eyes track an object moving across the visual field. ABNORMAL: eye cannot track at same rate and will not remain in center of orbit which suggests cerebellar dysfunction.
- Nystagmus assessment
- Positional nystagmus: test with Dix-Hallpike, Roll test or Sidelying Test (Semant Diagnostic Maneuver). NOTE–central causes of positional nystagmus do exist and will not respond to canalith repositioning
- Spontaneous Nystagmus: occurs from imbalance in vestibular signals being sent to oculomotor nerves. Leads to constant drift of eyes to one direction with brief corrections back the other way. Occurs after acute vestibular loss
-
- Peripheral lesion: fixing gaze on stable object will stop nystagmus, typically resolves within 24 hours.
- Central: nystagmus persists with fixation on nonmoving object
-
- Peripheral Nystagmus characteristics:
- Direction fixed and dominantly horizontal
- Suppressed with visual fixation
- More likely to be exacerbated when looking in direction of fast component
- Central Nystagmus characteristics
- Direction changing, more likely to be purely vertical or torsional
- Not diminished with fixation
- May be accompanied by one of the “D” symptoms: Diplopia, dysarthria, dysphagia, drop attacks, dyskinesia/ataxia (and muscle weakness on one side).
Put it into Practice
Now that you have a sense of what tests are available and what their results mean, keep an eye out for opportunities to practice them. Continuing education, online modules, textbooks and phone-a-neuro-therapist-friend are all great ways to build your confidence and knowledge in this area.


Leave a comment